Thanks to the advancement of lens technology, glasses lenses are no longer a single, one size fits all solution. There are a variety of different lens types that can be used in glasses, giving patients greater flexibility and control over their vision than ever before.
Single Vision Lenses
Also known as monovision lenses, these lenses are designed to correct the wearer’s vision at just one distance, and have a single prescription covering the entire surface of the lens. They are most often recommended for people who are either nearsighted (myopia) or farsighted (hyperopia) and who need glasses for a specific activity, such as driving or reading.
Progressive Lenses
Progressive lenses are multifocal lenses that can correct a patient’s vision at different working distances, ranging from far distance to reading distance. However, rather than designating different areas on the lenses for different distances with visible lines separating them, progressive lenses have a gradual change so that the wearer can smoothly transition from one lens power to another.
Bifocal and Trifocal Lenses
As you may have guessed from the name, bifocal and trifocal lenses have either two or three lens powers depending on which type you choose. Bifocal lenses support distance vision in the top half of the lens, and near vision in the lower half. Trifocal lenses support distance vision in the top third of the lens, intermediate vision in the middle segment and near vision in the bottom third. Whichever variety you choose, you will see visible lines separating each segment.
Bifocal and trifocal lenses are recommended for patients who are near or farsighted, and those who develop presbyopia, which is the natural hardening of the eye lens, that occurs as we get older. Presbyopia makes it harder for the lens of the eye to adapt to focus at different distances.
Multifocal Lenses
Multifocal lenses are the alternative name given to bifocal, trifocal and progressive lenses.

Clear Lens Extraction (CLE) is a surgical procedure that involves the removal of the natural lens of the eye and replacing it with an artificial lens implant, also known as an intraocular lens (IOL). CLE is primarily performed to correct refractive errors, such as nearsightedness, farsightedness, and astigmatism.
Understanding CLE and How It Works
Clear Lens Extraction is similar to cataract surgery, where the natural lens is removed and replaced with an IOL. However, in CLE, the lens is clear and not clouded as in the case of cataracts. The procedure begins with the administration of local anesthesia to numb the eye and ensure a painless experience for the patient.
Once the eye is numb, a small incision is made on the cornea, which is the clear front surface of the eye. Through this incision, your eye surgeon accesses the lens and carefully removes it. The artificial IOL is then inserted into the empty lens capsule. The IOL is specifically chosen to correct the patient's refractive error, providing them with improved vision.
After the IOL is implanted, the incision is closed with tiny sutures or self-sealing techniques. Following the surgery, patients are usually prescribed antibiotic and anti-inflammatory eye drops to prevent infection and reduce inflammation.
Factors to Consider Before Undergoing Clear Lens Extraction
Before deciding to undergo Clear Lens Extraction, there are several factors that need to be considered. Firstly, it is crucial to have a thorough eye examination to determine if you are a suitable candidate for the procedure. Your optometrist will evaluate your overall eye health and discuss your expectations and goals for vision correction.
Age is another important factor to consider. CLE is typically recommended for individuals over the age of 40 who have developed presbyopia, a condition that affects near vision. It is also important to have stable vision, as any changes in prescription can affect the accuracy of the IOL power calculation.
Additionally, it is essential to understand the potential risks and complications associated with the procedure. While CLE is generally safe, there is a small risk of infection, bleeding, and retinal detachment. Your optometrist will discuss these risks with you and address any concerns you may have.

In the realm of eye care, surgical co-management has emerged as a collaborative approach that aims to provide patients with comprehensive and seamless treatment. This concept involves the joint efforts of optometrists and ophthalmologists, each bringing their unique expertise to the table. By working together, these eye care professionals strive to enhance patient outcomes and deliver exceptional care.
The Role of Optometrist and Ophthalmologist in Surgical Co-Management
Surgical co-management is built upon the unique skill sets and areas of expertise of optometrists and ophthalmologists. By understanding their respective roles, you can appreciate the synergy that this collaborative approach fosters.
Optometrists are primary eye care professionals who specialize in the examination, diagnosis, and non-surgical treatment of vision disorders. Their responsibilities in surgical co-management include:
Performing comprehensive eye examinations and evaluations
Monitoring and managing pre-existing eye conditions
Providing pre-operative and post-operative care
Educating patients on surgical procedures and aftercare
Collaborating with ophthalmologists to ensure continuity of care
Ophthalmologists are medical doctors who specialize in the diagnosis, treatment, and surgical management of eye diseases and disorders. Their role in surgical co-management encompasses:
Evaluating patients' candidacy for surgical interventions
Performing complex surgical procedures
Providing specialized medical and surgical care
Collaborating with optometrists to ensure seamless patient care
Monitoring and managing post-operative complications
By combining the expertise of optometrists and ophthalmologists, surgical co-management ensures that patients receive comprehensive and coordinated care throughout their treatment journey.
How Surgical Co-Management Works
Surgical co-management is a well-orchestrated process that involves several key steps. Understanding how it works can help you navigate this collaborative approach with confidence.
Initial Evaluation: The process typically begins with an optometrist conducting a comprehensive eye examination. During this evaluation, the optometrist assesses the patient's visual needs, identifies any potential issues, and determines if a surgical intervention is necessary.
Referral and Consultation: If surgery is recommended, the optometrist refers the patient to an ophthalmologist for further evaluation and consultation. This step ensures that the patient receives specialized medical advice and a thorough assessment of their suitability for the proposed surgical procedure.
Pre-operative Care: The optometrist plays a crucial role in providing pre-operative care, which may include managing any existing eye conditions, ensuring the patient understands the surgical process, and addressing any concerns or questions they may have.
Surgical Procedure: The ophthalmologist performs the necessary surgical intervention, leveraging their specialized training and expertise in surgical techniques.
Post-operative Care: After the surgery, the patient's care transitions back to the optometrist, who closely monitors the recovery process and provides post-operative care and management. This may involve follow-up appointments, monitoring for any complications, and ensuring the patient adheres to the prescribed treatment plan.
Ongoing Collaboration: Throughout the entire process, the optometrist and ophthalmologist maintain open communication and collaborate closely. This ensures that the patient's care is seamless, and any concerns or issues are promptly addressed by the appropriate healthcare professional.

Optical Coherence Tomography is a non-invasive imaging test that may be performed as a standard part of your regular, comprehensive exams, or you may be able to request this test as an addition to your usual exam.
Optical Coherence Tomography uses light waves to take cross-section images of your retina, which is the area of light-sensitive cells at the back of your eye that is responsible for receiving light and transmitting it into messages that are sent up to the brain. The technology behind OCT enables your eye doctor to see each of the different layers that make up the retina. By being able to see these and measure them, they can obtain a much clearer picture of the overall health and condition of your eyes.
Why are Optical Coherence Tomography scans important?
When you choose to have an OCT scan at fairly regular intervals, such as during your normal comprehensive eye exams, your eye doctor can compare newer results to previous ones. This helps them to build up a picture of the health of your eyes, and spot any changes which may be concerning, early, before they cause symptoms or have a permanent effect on your vision.
Anyone can have an OCT scan, but they are particularly recommended for patients over the age of 25 who are concerned about the health of their eyes, or who are at risk of or already have diabetes, glaucoma or a family history of eye disease. This is because they can be used to spot the early signs of a range of eye diseases, including glaucoma, diabetic retinopathy, macular degeneration, disorders of the optic nerve and more – even before you realize that you are affected.

Dry eye is a common condition that affects millions of people worldwide. It occurs when the eyes do not produce enough tears or when the tears evaporate too quickly. This can lead to discomfort, irritation, and even vision problems. If you are suffering from the discomfort of dry eye, MiBo Thermoflo can offer you a revolutionary solution.
Understanding the Causes of Dry Eye
Dry eye is a condition that occurs when the eyes do not produce enough tears or when the tears evaporate too quickly. There are several factors that can contribute to this condition, including environmental factors, certain medications, and aging. Environmental factors such as dry or windy climates, air conditioning, and excessive screen time can all worsen dry eye symptoms. Additionally, certain medications like antihistamines, decongestants, and diuretics can decrease tear production. Aging is also a common cause of dry eye, as tear production naturally decreases as we get older.
Meibomian gland dysfunction (MGD) and blepharitis are two common conditions that can contribute to the development of dry eye. MGD occurs when the meibomian glands, which are responsible for producing the oily layer of tears, become blocked or dysfunctional. This can lead to an inadequate amount of oil in the tears, causing them to evaporate too quickly. Blepharitis is an inflammation of the eyelids that can disrupt the normal functioning of the meibomian glands.

Eye care professionals use Optikam’s technology to capture more than 3 million eyewear measurements every year. The OptikamPad iPad app is a total dispensing solution that enables eye care professionals to successfully assist patients at all stages of the eyewear dispensing process, providing them with a unique and custom patient experience.
Optikam Posture Devise (OPD)
You may be surprised to learn that wearing glasses can and likely will affect your posture. Glasses lenses are most accurate when you look directly through their center. This means if your glasses are sitting too low or have slipped down your nose, you may find that you are subconsciously tilting your head back and this can affect your overall posture.
Optikam’s OPD measurement device is a cutting-edge tool that obtains eyewear measurements that take into account how the frame will be worn by patients, enabling the fit to be customized to their individual parameters. The ten measurements taken into account when determining each patient’s position of wear include:
Monocular pupillary distance
Multifocal seg heights
Pantoscopic tilt
Rear vertex distance
Wrap (face form tilt)
Near pupillary distance
This results in frames that not only look fantastic, but that also fit perfectly, remaining both comfortable and stable on the face without you needing to adopt an unnatural posture. The measurements obtained by the Optikam OPD measurement tool are immediately visible on your eye doctor’s tablet so that they can recommend which alterations to the frames are needed to ensure that the frames fit with precision and gives you the best visual experience.

Presbyopia is a natural and inevitable part of aging that affects the eyes' ability to focus on close objects. Unlike other vision conditions, presbyopia isn’t caused by the shape of the eye or structural abnormalities but is instead a result of the eye’s lens losing its flexibility over time.
What is Presbyopia?
Presbyopia is a refractive error, meaning it affects how the eyes bend (or refract) light to focus it on the retina. Unlike nearsightedness (myopia) or farsightedness (hyperopia), which are caused by the shape of the eyeball or cornea, presbyopia is due to the aging of the eye's lens. Over time, the lens becomes less flexible, making it difficult to focus on nearby objects. Presbyopia isn’t a disease or an abnormality—it’s simply a natural consequence of the aging process.
What Causes Presbyopia?
The lens inside the eye changes shape to focus light on the retina, allowing us to see clearly at varying distances. When viewing nearby objects, the lens thickens and curves to increase its refractive power.
As we age, however:
Lens Stiffening: The lens loses elasticity, making it harder to bend and adjust for near vision.
Weakened Ciliary Muscles: The muscles that help change the shape of the lens may lose their strength over time, further reducing the eye’s ability to focus on close objects.
Structural Changes: The lens also grows thicker and less transparent with age, which contributes to reduced focusing ability.
These changes are gradual, typically starting in a person’s 30s and becoming noticeable by their early to mid-40s.
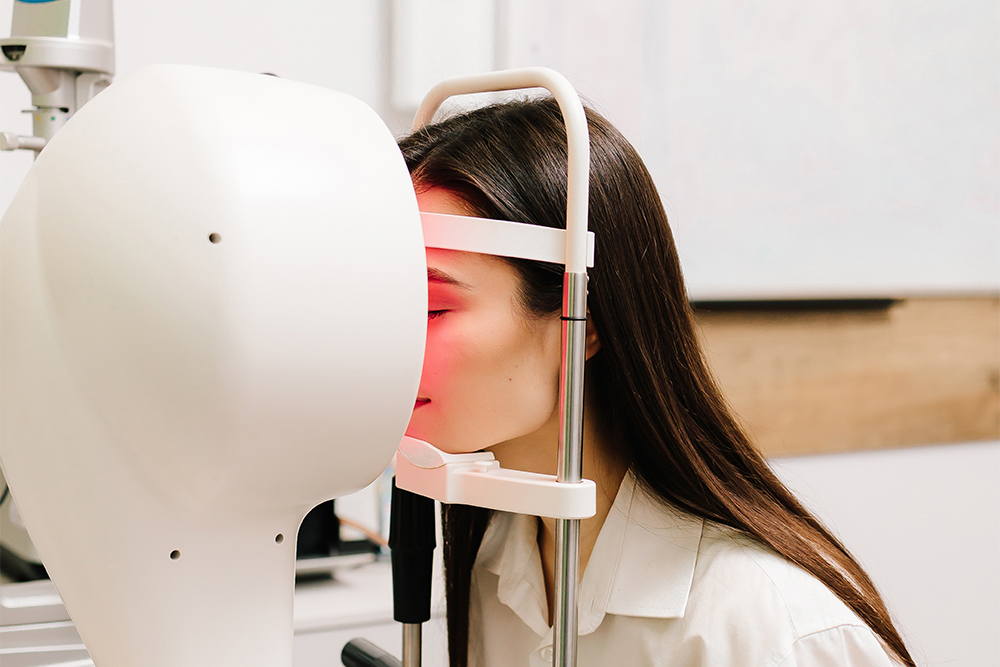
When it comes to diagnosing and managing complex vision conditions, precision matters. One of the most advanced tools is Medmont topography - a state-of-the-art technology that provides highly detailed maps of the cornea. Whether you are being evaluated for specialty contact lenses, dry eye treatment, or refractive surgery, Medmont topography plays a critical role in delivering accurate, customized care.
What Is Medmont Topography?
Medmont topography refers to corneal imaging performed with the Medmont E300 Corneal Topographer, a diagnostic device designed to capture detailed curvature measurements of the cornea.
Using advanced Placido disc technology, the system projects illuminated rings onto the cornea and analyzes their reflections. From this data, it generates a color-coded map that reveals the shape, elevation, and curvature of the cornea with exceptional accuracy.
Why Is Corneal Topography Important?
The cornea is responsible for approximately two-thirds of the eye’s focusing power. Even subtle irregularities can significantly affect vision. Medmont topography allows your eye doctor to detect and monitor:
Keratoconus and other corneal ectasias
Corneal irregularities or scarring
Post-surgical corneal changes
Astigmatism patterns
Contact lens fitting complications
Early signs of corneal distortion
Because it provides highly detailed imaging, Medmont topography often identifies changes long before they become noticeable in a routine vision exam.
How Medmont Topography Improves Contact Lens Fitting
For patients who require specialty contact lenses - such as scleral lenses, hybrid lenses, or lenses for keratoconus - precise corneal mapping is essential.
The Medmont system offers:
High-resolution curvature data
Wide corneal coverage
Repeatable, reliable measurements
Advanced software analysis
This allows your doctor to design and fit custom lenses with greater accuracy, improving comfort, stability, and visual clarity while reducing trial-and-error fittings.
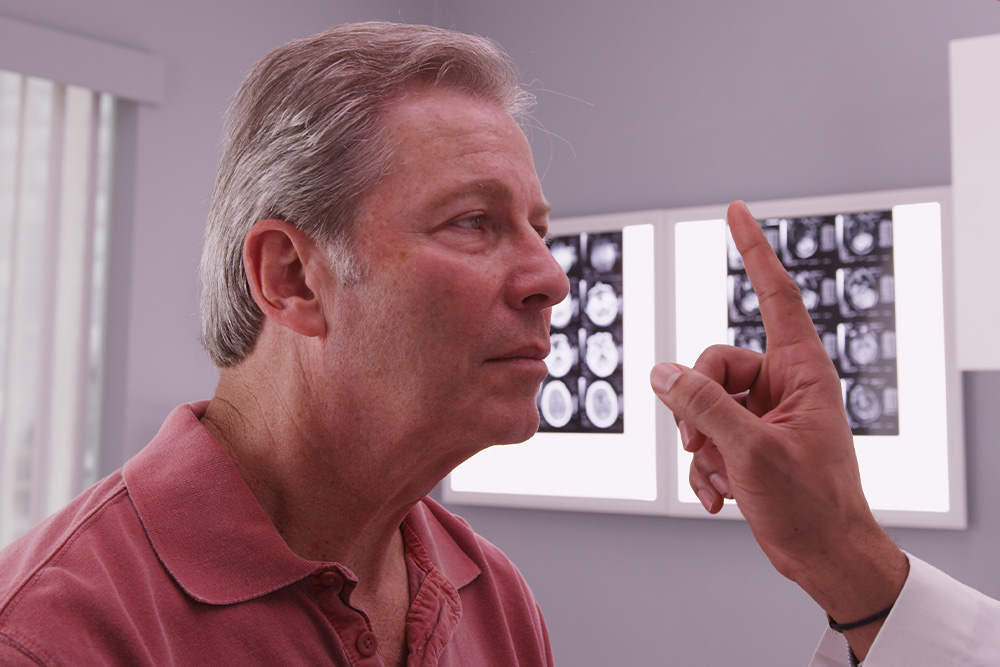
Neuro-Optometric Rehabilitation
When most people think about vision problems, they picture issues with the eyes themselves. However, many visual difficulties actually begin in the brain. After a concussion, stroke, or other brain injury, the connection between the eyes and brain can be disrupted - causing symptoms that affect balance, reading, focus, and even daily comfort.
Brain Injuries and Vision
Your visual system is complex - about 70% of the brain is involved in vision processing. After a traumatic brain injury (TBI), concussion, or neurological event such as a stroke, the pathways that coordinate eye movement, focus, and perception can become impaired.
This can result in symptoms such as:
Blurred or double vision
Eye strain and headaches
Difficulty reading or focusing
Dizziness or balance problems
Light sensitivity
Problems with depth perception
These visual issues often persist long after other symptoms of a brain injury have improved, making specialized vision care essential for recovery.
What Is Neuro-Optometric Rehabilitation?
Neuro-optometric rehabilitation is a specialized form of vision therapy designed to retrain how the brain and eyes work together. Unlike traditional eye care that focuses on eyesight alone, this therapy targets the neurological processes behind vision. Our doctor evaluates how the eyes and brain communicate and creates a personalized treatment plan to rebuild these visual pathways. The goal is to restore comfort, coordination, and clarity - improving overall visual function and quality of life.

Newton™
Newton™, formerly Neurolens®, is the first and only prescription lenses that include an element of contoured prism in their design. This prism is designed to bring the patient’s eyes into more equal alignment, and this should help to provide relief from the symptoms that are associated with several eye misalignment conditions, including digital eye strain and binocular vision dysfunction.
What is digital eye strain?
Digital eye strain is the name given to describe a group of symptoms that can occur when someone spends long periods of time using digital devices. Since using digital devices requires the eyes to work harder than normal and we don’t always position our devices the perfect distance away, it can lead to issues such as eye pain, dry and irritated eyes, eye fatigue, light sensitivity, and blurred vision. Unsurprisingly, the number of people who are experiencing digital eye strain has grown significantly over the last few years and is expected to continue to do so.
What is binocular vision dysfunction?
Binocular vision dysfunction, also known as BVD for short, is another eye condition but is one that is very misunderstood. Binocular vision dysfunction occurs when the eyes aren’t perfectly aligned, causing your brain and eyes to work harder than normal in order to create a clear visual image and remain focused. This places pressure on the trigeminal nerve, which is the nerve that is responsible for the majority of the sensations that we experience in our head and back. BVD can often manifest as other things owing to the huge range of symptoms that are associated with the condition. These can include, but aren’t limited to:
Blurred vision
Headaches/migraines
Double vision
Motion sickness
Vertigo
Dizziness
Anxiety
Many people don’t think to visit an eye doctor when they are experiencing these symptoms, but all can occur simply because the eyes are out of alignment.